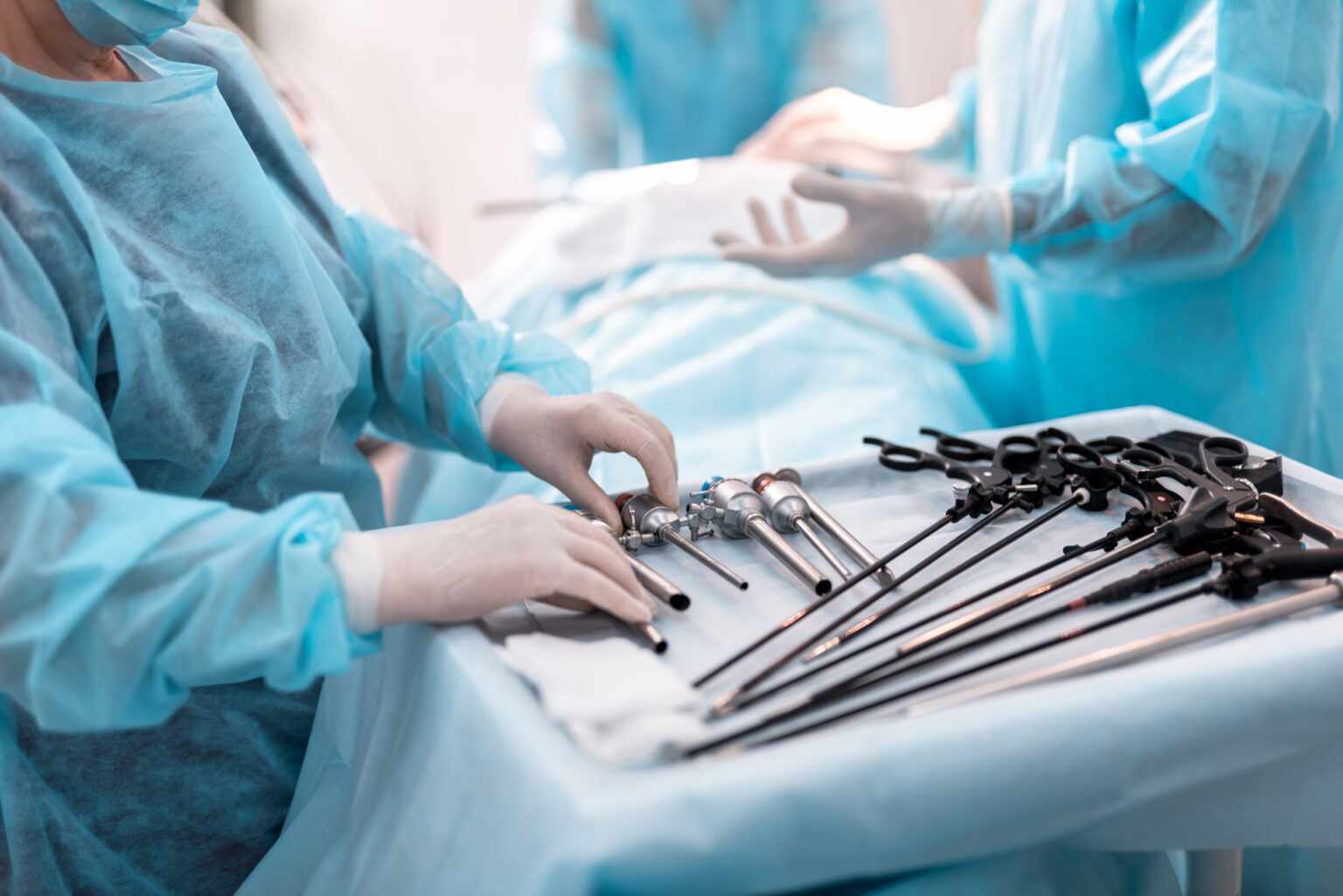
Laparoscopy can help diagnose a fertility problem. Laparoscopy surgery for infertility is performing tiny incisions in the abdomen and inserting a laparoscope or a fiber-optic tube, having a camera and light, to examine the pelvic cavity and reproductive organs by the surgeon. With laparoscopy, a surgeon not only looks closely over the abdomen organs but also repairs them.
Performed under local anesthetic, a laparoscopic procedure generally takes about 45- 60 minutes. By inflating the abdomen using gas, which is either carbon dioxide or nitrous oxide, to make the abdomen organs visible by having them moved away from the abdominal wall, the surgeon inserts the laparoscope into the tiny incisions. The camera captures the images of the internal organs in the pelvic cavity, and displays them on a video screen.
The laparoscopic surgery is advised for the following possible causes of infertility such as scar tissue, endometriosis, abnormalities in the ovaries and uterus, fibroid tumors, and blocked fallopian tubes. The surgeon performs an operative laparoscopy to correct the problems by removing endometrial tissue, fibroids, or scar tissue using small surgical instruments. Once the tissue is removed using electric current or a laser beam, the surgical incision is closed using clips or stitches.
Also Read: Signs of Miscarriage
Is Laparoscopy Surgery for Infertility Recommended?
The argument against performing laparoscopic surgery for infertility in women is still going on, and in most cases, doctors recommend surgery for women who are experiencing pelvic pain. Despite the introduction of in vitro fertilization (IVF), as well as the assisted reproductive technologies’ (ART) improved success rates, the use of laparoscopic surgery as a solution for infertility is still recommended.
When the unexplained infertility is a challenge, even after the successful use of IVF technology, the controversy over the use of laparoscopic diagnostic still majorly rests on women with endometriosis, history of tubal sterilization, ectopic pregnancy, tubal adhesions, and uterine fibroids blocking or distorting the uterine cavity. However, there is risk of pelvic adhesions owing to the use of a hysterosalpingogram HSG to check the patency of the fallopian tubes, and the adhesions can be confirmed only by laparoscopic surgery.
Similarly, laparoscopic surgery, especially laparoscopic ovarian drilling (LOD) could be the most advisable treatment option for women with a common health problem like polycystic ovary syndrome (PCOS). With good ovarian reserve, such patients are generally resistant to clomiphene citrate. When the procedure helps improve the hormonal milieu and induce mono-follicular development, it eliminates the chances of developing ovarian hyperstimulation syndrome and reduces the multiple pregnancy rate.
Diagnostic laparoscopy is essential to diagnose mild endometriosis in women and the laparoscopy excision is commonly performed to treat endometriosis by removing lesions; thus, increasing pregnancy rates. Laparoscopy may be recommended by your doctor for all the above medical issues.
Also, Read: Diagnostic Hysterolaparoscopy
What Are the Risks of Laparoscopy?
Laparoscopy for infertility has risks like any surgery. There are minor and major complications though only 1 or 2 patients out of 100 who undergo laparoscopy for treating infertility experience them. The most common complications are viewed minor ones, and they include:
- Skin irritation or skin rashes around the incision area
- Bladder infection (cystitis)
Severe complications post the laparoscopic surgery are less common ones, and they include:
- Hematomas or seromas (collection of blood under the skin and outside of the blood vessel
- Formation of adhesions
- Nerve damage
- Allergic reaction
- Blood clots
- Urinary retention
Some research studies have proved that using laparoscopy to remove endometrial polyps helps improve fertility, as well as increases the chances of pregnancy, despite the number or size of the polyps. The American Association of Laparoscopic Surgeons (AAGL) in the practice guidelines has recommended surgical removal of a polyp in any infertile patient for there is a greater chance for the natural conception or assisted reproductive technology (ART) to be successful.
Similarly, a review of the studies related to uterine fibroids and fertility revealed that the women with submucosal fibroids have decreased fertility outcomes, and removing the fibroids may help conception. The in vitro fertilization (IVF) outcomes have shown improvement by 50 percent when dilated fallopian tubes were removed using laparoscopy, and hence, the treatment is highly recommended.
However, several infertility specialists today favor ART and is bypassing diagnostic laparoscopy owing to its requirement of general anesthesia, which they associate with a low yet presumably serious incidence of complications and risks. Despite this, laparoscopy still plays an important role in a small but considerable percentage of infertile women.
In conclusion, the laparoscopy surgery can be considered boon in some cases for its critical role in the treatment of infertility. There are a considerable number of women with infertility and among them those with a PCOS, tubal factor and unexplained infertility are highly benefitted from the surgery. In the cases of IUI/IVF procedures such as salpingectomy, ablation of endometriosis and lysis of adhesions during laparoscopy, the conception chances for women with infertility are found high.
Also Read: Yoga for a move from Infertility towards Pregnancy